Cardiovascular disease (CVD) is the world’s leading cause of death, claiming millions of lives annually. But what exactly is cardiovascular disease, and how can it be prevented? If you’re concerned about heart health or want to protect your loved ones, understanding this condition is crucial.
Heart disease, strokes, and other cardiovascular conditions often develop silently, putting you at risk without any obvious warning signs. But with the right knowledge, you can identify risk factors early, recognize symptoms, and take proactive steps to safeguard your health.
Learn what is cardiovascular disease, its types, symptoms, risk factors, diagnosis, treatment options, and preventive measures.
What is Cardiovascular Disease?
Cardiovascular disease refers to a group of disorders that affect the heart and blood vessels. These conditions include coronary artery disease, heart attacks, strokes, arrhythmias, and more. CVD disrupts the normal flow of blood through the cardiovascular system, leading to life-threatening complications and a diminished quality of life.
The cardiovascular system consists of the heart and an intricate network of blood vessels, including arteries, veins, and capillaries. When any part of this system is impaired, it can result in a range of symptoms and health issues, affecting not only your heart but also other vital organs.
CVD is often a result of plaque buildup in the arteries, which restricts blood flow. Over time, this plaque can harden (a condition known as atherosclerosis), leading to heart attacks, strokes, and other serious complications.
Globally, CVD is a major health concern, affecting millions of people each year. It is not limited to a particular age group or demographic and can strike without warning, making awareness and early detection critical. Knowing what cardiovascular disease is and how it develops is the first step toward prevention and management.
Types of Cardiovascular Disease
Cardiovascular disease (CVD) is an umbrella term that includes several conditions affecting the heart and blood vessels. Understanding these different types is essential for recognizing symptoms, understanding treatment options, and taking preventive measures.
Below are the main types of cardiovascular disease:
1. Coronary Artery Disease (CAD)
Coronary artery disease, also known as coronary heart disease, is the most common form of cardiovascular disease. It occurs when the coronary arteries become narrowed or blocked due to the buildup of plaque, which consists of cholesterol, fatty substances, cellular waste products, and calcium. This process is known as atherosclerosis.
- Symptoms: Individuals may experience angina, which manifests as chest pain or discomfort, often triggered by physical exertion or emotional stress. The pain can be described as pressure, squeezing, or fullness in the chest.
- Complications: If a coronary artery becomes completely blocked, it can lead to a heart attack (myocardial infarction). In this event, the heart muscle is deprived of oxygen and can suffer damage or death.
2. Heart Attack (Myocardial Infarction)
A heart attack occurs when blood flow to a part of the heart muscle is blocked for an extended period. This blockage can happen due to a blood clot forming on the surface of a ruptured plaque within a coronary artery.
- Symptoms: Common symptoms of a heart attack include:
- Chest Pain or Discomfort: Often described as a feeling of pressure, tightness, or a heavy weight on the chest.
- Radiating Pain: Pain or discomfort may spread to the shoulders, neck, arms, back, teeth, or jaw.
- Shortness of Breath: This may occur with or without chest discomfort and can be experienced during rest or physical activity.
- Other Signs: These can include cold sweat, nausea, and lightheadedness.
Timely medical intervention is crucial in minimizing heart damage and improving outcomes.
3. Stroke
Strokes occur when the blood supply to the brain is interrupted or reduced, preventing brain tissue from getting necessary nutrients and oxygen. There are two primary types of strokes:
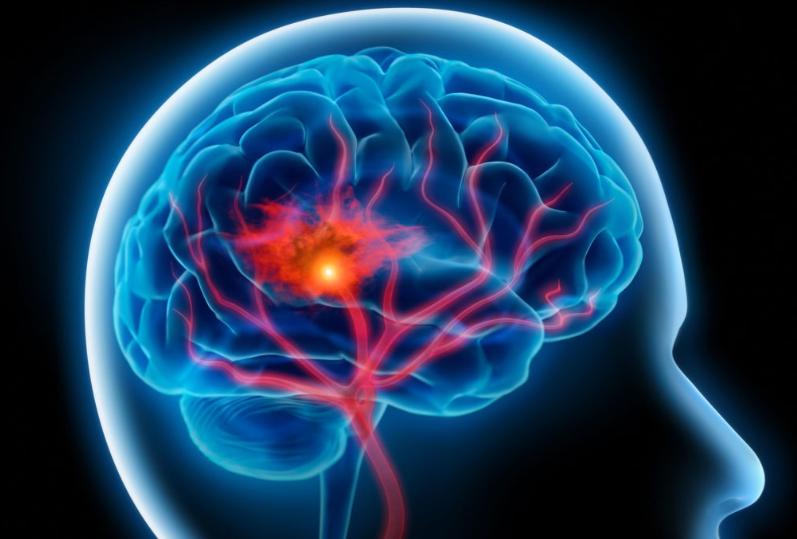
- Ischemic Stroke: This is the most common type, accounting for about 87% of all strokes. It occurs when a blood vessel supplying blood to the brain is blocked, often by a blood clot. This can happen in two ways:
- Thrombotic Stroke: A blood clot forms in an artery supplying blood to the brain.
- Embolic Stroke: A blood clot forms elsewhere in the body (often in the heart) and travels to the brain.
- Hemorrhagic Stroke: This occurs when a blood vessel in the brain ruptures, leading to bleeding. This type can be caused by conditions like high blood pressure, aneurysms, or arteriovenous malformations.
- Symptoms: Common symptoms of a stroke can include sudden numbness or weakness (especially on one side of the body), confusion, difficulty speaking, vision problems, severe headache, and trouble walking or balancing.
Recognizing the signs of a stroke and seeking immediate medical attention can significantly improve outcomes.
4. Heart Failure
Heart failure, also known as congestive heart failure, occurs when the heart is unable to pump blood effectively to meet the body’s needs. This condition can be caused by various factors, including CAD, high blood pressure, and previous heart attacks.
- Symptoms:
- Fatigue: Individuals may feel excessively tired or weak, even with minimal exertion.
- Fluid Retention: This can lead to swelling in the legs, ankles, feet, or abdomen due to fluid buildup.
- Breathing Difficulties: Shortness of breath may occur during physical activity or when lying flat. People with heart failure might also experience coughing or wheezing.
- Types of Heart Failure:
- Left-Sided Heart Failure: The left side of the heart cannot pump enough blood to the body. This can lead to fluid accumulation in the lungs.
- Right-Sided Heart Failure: The right side of the heart cannot pump blood to the lungs, leading to fluid buildup in the abdomen and legs.
5. Arrhythmias
Arrhythmias are irregular heartbeats that can occur when the heart’s electrical signals malfunction. They can cause the heart to beat too quickly (tachycardia), too slowly (bradycardia), or erratically.
- Common Types:
- Atrial Fibrillation (AFib): A common type of arrhythmia characterized by a rapid and irregular heartbeat. AFib increases the risk of stroke and other heart-related complications.
- Ventricular Tachycardia: A fast heart rate originating from the lower chambers of the heart. It can be life-threatening if it persists for more than a few seconds.
- Symptoms: Some people may experience palpitations (a sensation of fluttering in the chest), dizziness, fainting, or chest pain, while others may not notice any symptoms at all.
6. Peripheral Artery Disease (PAD)
Peripheral artery disease occurs when the blood vessels that supply blood to the limbs become narrowed or blocked, typically due to atherosclerosis. This reduced blood flow can lead to pain and other complications.
- Symptoms: The most common symptom is leg pain, often described as cramping or heaviness during physical activity, such as walking or climbing stairs. This pain typically subsides with rest.
- Complications: PAD increases the risk of more severe cardiovascular events, such as heart attack and stroke, and can lead to critical limb ischemia, where blood flow is severely restricted.
7. Congenital Heart Disease
Congenital heart disease refers to structural heart defects present at birth. These defects can affect the heart’s walls, valves, or blood vessels, impacting normal blood flow.
- Types of Defects:
- Septal Defects: Holes in the heart’s septum (the wall dividing the left and right sides of the heart).
- Valvular Defects: Malformations of the heart valves that affect blood flow through the heart.
- Symptoms: Symptoms can vary widely based on the type and severity of the defect but may include cyanosis (a bluish tint to the skin, lips, and nails), difficulty breathing, and poor feeding in infants.
Causes and Risk Factors of Cardiovascular Disease
Understanding the causes and risk factors of cardiovascular disease is crucial for prevention and early intervention. The factors can be classified into modifiable and non-modifiable risk factors.
Modifiable Risk Factors
These are lifestyle factors that individuals can control or change:
- Unhealthy Diet: Consuming a diet high in saturated fats, trans fats, cholesterol, and sodium can lead to high cholesterol levels and hypertension. Focus on a diet rich in:
- Fruits and Vegetables: Provide essential vitamins, minerals, and fiber while being low in calories.
- Whole Grains: Oats, quinoa, and whole wheat can help lower cholesterol levels.
- Lean Proteins: Chicken, fish, and plant-based proteins such as legumes are healthier choices compared to red and processed meats.
- Physical Inactivity: A sedentary lifestyle can lead to obesity, high blood pressure, and poor cardiovascular health. Engaging in regular physical activity strengthens the heart, improves circulation, and enhances overall well-being. The American Heart Association recommends at least:
- 150 minutes of moderate aerobic activity (like brisk walking) or
- 75 minutes of vigorous activity (like running) each week, along with muscle-strengthening exercises on two or more days.
- Smoking: Tobacco use is a significant risk factor for cardiovascular disease. It damages the lining of blood vessels, reduces oxygen supply, and promotes plaque buildup. Quitting smoking can lead to immediate health benefits, including:
- Improved circulation.
- Decreased heart rate.
- Lowered risk of heart disease and stroke.
- Excessive Alcohol Consumption: Drinking alcohol in moderation can be acceptable, but excessive consumption can lead to high blood pressure, heart failure, and increased calorie intake leading to weight gain. Guidelines suggest limiting alcohol to:
- One drink per day for women and
- Two drinks per day for men.
- High Blood Pressure (Hypertension): Chronic hypertension exerts excessive force on artery walls, leading to heart damage. Regular monitoring, lifestyle changes, and medications (if prescribed) are vital for managing blood pressure.
- High Cholesterol: Elevated levels of LDL (bad) cholesterol contribute to plaque buildup, while low levels of HDL (good) cholesterol are protective. Regular screenings and a heart-healthy diet can help manage cholesterol levels.
- Diabetes: Uncontrolled diabetes increases the risk of cardiovascular disease due to damage to blood vessels and nerves. Managing blood sugar levels through diet, exercise, and medication is crucial for reducing heart disease risk.
- Obesity: Excess weight, especially around the abdomen, increases the likelihood of hypertension, high cholesterol, and diabetes. A combination of a balanced diet and regular physical activity is essential for achieving and maintaining a healthy weight.
- Chronic Stress: Prolonged stress can lead to unhealthy coping mechanisms (e.g., overeating, smoking) and can elevate blood pressure. Effective stress management techniques, such as mindfulness, meditation, and yoga, can mitigate stress’s impact on heart health.
Non-Modifiable Risk Factors
These are factors that individuals cannot change:
- Age: The risk of cardiovascular disease increases with age. Men over 45 and women over 55 are at higher risk due to changes in blood vessels and the heart’s structure.
- Gender: Generally, men have a higher risk of heart disease at a younger age compared to women. However, post-menopause, women’s risk increases due to hormonal changes.
- Family History: A family history of heart disease can elevate an individual’s risk, particularly if close relatives had cardiovascular issues at a young age. Genetics can influence cholesterol levels, blood pressure, and overall heart health.
- Ethnicity: Certain ethnic groups may have a higher predisposition to cardiovascular diseases due to genetic, environmental, and lifestyle factors. For instance, African Americans often face higher rates of hypertension and heart disease compared to Caucasian Americans.
Symptoms of Cardiovascular Disease
Recognizing the symptoms of cardiovascular disease early can be lifesaving. Symptoms vary depending on the specific condition but often share common signs:
General Symptoms
- Chest pain or discomfort (angina)
- Shortness of breath
- Fatigue, especially during physical exertion
- Nausea or vomiting
- Dizziness or lightheadedness
Symptoms of a Heart Attack
- Intense, crushing chest pain that may spread to the arms, neck, or jaw.
- Shortness of breath, nausea, and cold sweats.
- Lightheadedness or dizziness.
- Unexplained fatigue, particularly in women.
Symptoms of a Stroke
- Face drooping on one side.
- Arm weakness, often on one side.
- Speech difficulty, such as slurring or inability to speak.
- Time to call emergency services—act quickly to prevent permanent damage.
Heart Failure Symptoms
- Swelling in the legs and ankles.
- Persistent coughing or wheezing.
- Rapid or irregular heartbeat.
- Increased need to urinate at night.
Peripheral Artery Disease Symptoms
- Leg pain or cramping during physical activities like walking or climbing stairs.
- Numbness or weakness in the legs.
- Coldness in the lower leg or foot, especially when compared to the other side.
- Sores on the toes, feet, or legs that won’t heal.
How is Cardiovascular Disease Diagnosed?
Diagnosing cardiovascular disease involves a combination of medical history, physical examination, and diagnostic tests. Early diagnosis and intervention are key to preventing complications.
Physical Examination
During a physical exam, your doctor will check for symptoms such as high blood pressure, elevated cholesterol levels, and family history of heart disease. They may also listen to your heart and lungs to detect abnormal sounds or rhythms.
Electrocardiogram (ECG)
An electrocardiogram measures the heart’s electrical activity and can detect abnormalities in the heart’s rhythm and structure. It is a simple, non-invasive test that can reveal if the heart is enlarged or overworked.
Echocardiogram
This test uses sound waves to create images of the heart’s structure and function. It can assess the size and shape of the heart, as well as how well the chambers and valves are functioning.
Blood Tests
Blood tests can provide critical information about cholesterol levels, blood sugar, and other markers that indicate heart health. Elevated levels of certain proteins, such as troponin, can signal heart damage.
Stress Test
A stress test measures the heart’s ability to function during physical exertion. This test is often performed on a treadmill or stationary bike and helps identify blood flow problems.
Coronary Angiography
This procedure uses X-ray imaging to examine the coronary arteries. It involves injecting a contrast dye into the blood vessels to highlight blockages or narrowing that could indicate coronary artery disease.
Treatment Options for Cardiovascular Disease
The treatment plan for cardiovascular disease depends on the specific condition, severity, and individual health factors. Treatment options include:
1. Lifestyle Changes
Adopting a heart-healthy lifestyle is the first step in managing cardiovascular disease. This includes maintaining a balanced diet rich in fruits, vegetables, and whole grains, engaging in regular physical activity, quitting smoking, and limiting alcohol intake.
2. Medications
Medications are often prescribed to control blood pressure, lower cholesterol levels, prevent blood clots, and manage symptoms. Common medications include:
- Statins: Used to lower cholesterol levels.
- Beta-blockers: Reduce blood pressure and decrease the heart’s workload.
- Anticoagulants: Prevent blood clot formation.
- ACE Inhibitors: Lower blood pressure by relaxing blood vessels.
3. Medical Procedures and Surgery
In severe cases, surgical interventions may be necessary to restore blood flow or repair heart damage:
- Angioplasty and Stent Placement: A procedure that opens narrowed arteries using a balloon and a small wire mesh tube called a stent.
- Coronary Artery Bypass Surgery (CABG): Creates a new pathway for blood to flow to the heart by using blood vessels from other parts of the body.
- Heart Transplant: In cases of end-stage heart failure, a heart transplant may be considered.
Preventing Cardiovascular Disease
Preventive measures can significantly reduce the risk of developing cardiovascular disease. Here are some effective strategies:
- Maintain a Heart-Healthy Diet:
- Focus on Nutrition: Prioritize fruits, vegetables, whole grains, lean proteins, and healthy fats (like olive oil and nuts).
- Limit Processed Foods: Reduce the intake of foods high in sugar, salt, and unhealthy fats.
- Stay Hydrated: Drink plenty of water and limit sugary drinks.
- Regular Physical Activity:
- Establish a Routine: Aim for at least 150 minutes of moderate-intensity aerobic exercise each week.
- Incorporate Variety: Include activities you enjoy, such as dancing, swimming, or hiking, to maintain motivation.
- Quit Smoking:
- Seek Support: Utilize resources such as smoking cessation programs or counseling services to help quit.
- Avoid Secondhand Smoke: Protect yourself from exposure to tobacco smoke, which can also harm cardiovascular health.
- Limit Alcohol Intake:
- Practice Moderation: Stick to recommended guidelines for alcohol consumption to protect heart health.
- Manage Stress:
- Monitor Blood Pressure and Cholesterol Levels:
- Regular Check-ups: Schedule regular visits with your healthcare provider to monitor heart health indicators.
- Adhere to Medication: If prescribed medication for hypertension or high cholesterol, take it as directed.
- Diabetes Management:
- Regular Screenings: Monitor blood sugar levels and follow a diabetes management plan, including a balanced diet and regular exercise.
- Weight Management:
- Set Realistic Goals: Work toward a healthy weight through diet and exercise. Even a modest weight loss can significantly reduce heart disease risk.
- Stay Informed:
- Educate Yourself: Stay aware of the latest cardiovascular health information and risk factors. Knowledge empowers you to make healthier choices.

Cardiovascular disease is a serious health concern that can have devastating effects if left unchecked. However, understanding what it is, its types, risk factors, and treatment options gives you the power to take control of your heart health.
Take proactive measures to protect yourself and your loved ones by adopting a heart-healthy lifestyle today. Prevention and early intervention are your best defenses against this silent killer. Stay informed, stay healthy, and keep your heart strong.


7 Comments